Setting the Stage: Why Point‑of‑Care Testing Matters Today
Point‑of‑care testing (POCT) delivers diagnostic results at or near the patient’s side within minutes, eliminating the need for sample transport to a central laboratory. This rapid turnaround enables clinicians to make treatment decisions during a single visit, reducing hospital stays, repeat appointments and overall care costs. Faster results improve patient outcomes by allowing immediate initiation of therapy—e.g., same‑day antiretroviral treatment for HIV or early sepsis management—and increase satisfaction, especially in underserved or remote communities. POCT aligns with global health initiatives such as the WHO’s ASSURED/REASSURED criteria and India’s National Health Policy, Ayushman Bharat, and NHS Long‑Term Plan, which all emphasize decentralized, affordable diagnostics to expand access, enhance disease surveillance, and support patient‑centric care.
Speed and Convenience: The Clinical Edge of Rapid Diagnostics

Point‑of‑care testing (POCT) shrinks diagnostic turnaround from hours or days to a few minutes, allowing clinicians to act during a single patient encounter. In diabetes care, handheld glucometers and HbA1c POCT devices report glucose levels within seconds, supporting immediate insulin adjustments and reducing the need for repeat laboratory visits. Infectious‑disease POCT—such as COVID‑19 antigen tests, HIV rapid assays, and malaria lateral‑flow kits—delivers results in under 30 minutes, enabling same‑day treatment initiation and infection control. Pediatric settings benefit from rapid viral panels and bedside complete‑blood‑count analyzers that differentiate bacterial from viral illnesses in four minutes, cutting unnecessary antibiotic use and hospital admissions. These speed gains translate into higher patient satisfaction: families avoid multiple appointments, travel costs drop, and clinicians see shorter clinic stays. Studies from the NHS Long‑Term Plan and Indian home‑collection models (e.g., Agam Diagnostics) demonstrate that rapid, on‑site results improve adherence, lower overall care costs, and bring quality diagnostics closer to where patients live.
A Global Market on the Rise

The point‑of‑care testing (POCT) market is set to explode, with forecasts valuing it at Global POCT market projected to grow from USD 44.48 billion in 2025 to USD 125.33 billion by 2034 (CAGR 12.20%). Asia‑Pacific expected to register the fastest CAGR (~12.38%) as rapid digitisation of health services, growing demand for decentralized diagnostics, and governmental pushes for patient‑centric care converge. Core multinational players continue to dominate the landscape: Abbott, Roche, and Siemens each supply a broad portfolio ranging from handheld glucose meters to cartridge‑based molecular platforms, leveraging AI‑driven analytics and cloud‑connectivity to meet the WHO REASSURED criteria. At the same time, a vibrant wave of start‑ups is emerging, capitalising on micro‑fluidics, nanomaterial biosensors and smartphone‑linked read‑outs to deliver low‑cost, multiplexed panels for infectious disease, chronic‑disease monitoring. This blend of established giants and innovative newcomers is reshaping the diagnostic ecosystem, accelerating the shift from centralized laboratories to near‑patient testing worldwide.
India’s Accelerating POCT Landscape
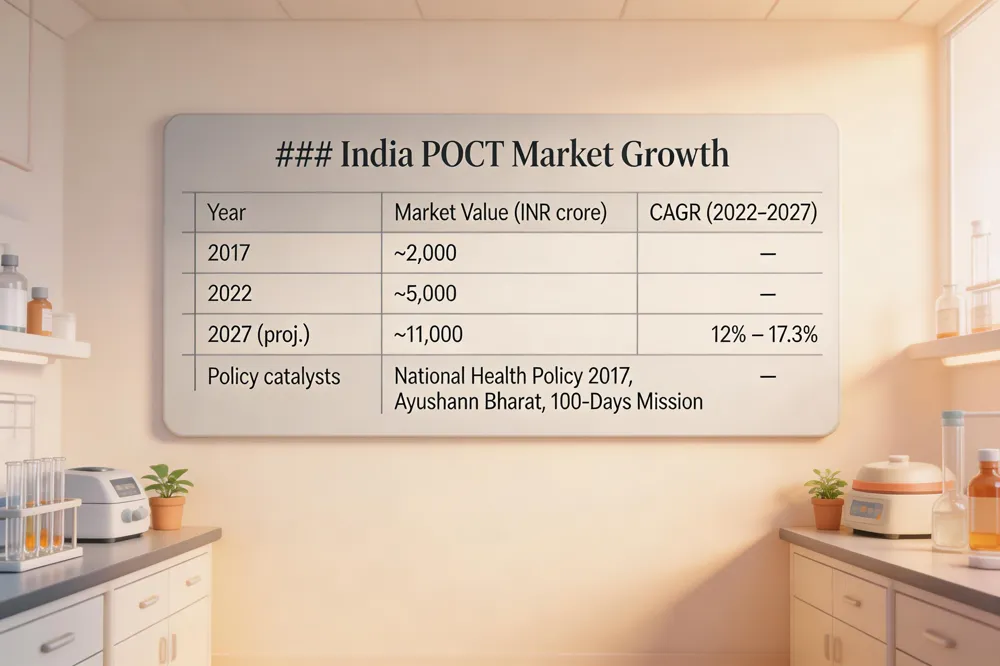

India’s point‑of‑care testing (POCT) market has expanded dramatically over the past decade. In 2017 the sector was valued at roughly INR 2,000 crore, and by 2022 it had risen to about INR 5,000 crore. Forecasts indicate a steep trajectory, with projected revenues of INR 11,000 crore by 2027. Depending on the source, the compound annual growth rate (CAGR) for the period 2022‑2027 ranges from 12 % to 17.3 %, reflecting robust demand for rapid, decentralized diagnostics. Government initiatives are a key catalyst behind this growth. The National Health Policy 2017 and the Ayushman Bharat programme prioritize affordable, community‑based health services, explicitly encouraging the deployment of POCT devices to reach underserved populations. Additionally, the 100‑Days Mission—aimed at rapid pandemic response—has underscored the need for fast, point‑of‑care diagnostics, further accelerating investment and adoption across both public and private health sectors.
Technology Trends Powering the Next Generation of POCT

The rapid evolution of point‑of‑care testing (POCT) is driven by a convergence of miniaturized electronics, microfluidics, and artificial‑intelligence/machine‑learning (AI/ML) integration. Tiny sensor chips and low‑power processors enable handheld devices that perform complex assays with a few drops of blood, urine, or saliva, while microfluidic channels automate sample handling, reduce reagent volumes, and improve assay robustness. AI/ML algorithms now interpret raw signal data in real time, flagging abnormal values, suggesting next‑step actions, and reducing reliance on highly trained operators.
Molecular POCT platforms have also leapt forward. Loop‑mediated isothermal amplification (LAMP) eliminates the need for thermal‑cycling, delivering nucleic‑acid detection at a constant temperature and enabling cartridge‑based PCR systems that provide results in under an hour. Multiplex lateral flow immunoassays (LFIA) can simultaneously detect several disease markers—such as viral antigens and cardiac biomarkers—on a single strip, expanding the clinical scope of rapid testing.
Finally, real‑time connectivity and adherence to the REASSURED criteria are reshaping deployment. Devices now embed Bluetooth or Wi‑Fi modules that push results directly to electronic health records, tele‑medicine platforms, and public‑health dashboards, ensuring rapid clinical decision‑making and surveillance. Wearable sensors, coupled with cloud‑based analytics, allow continuous monitoring of biomarkers like glucose or cardiac troponin, turning POCT into a proactive, personalized health tool that meets the WHO’s standards for affordability, sensitivity, specificity, and ease of use.
Regulatory and Quality Assurance Frameworks

The rapid growth of point‑of‑care testing (POCT) is underpinned by stringent regulatory and quality frameworks that guarantee reliable results at the patient’s side. Internationally, the WHO’s ASSURED (Affordable, Sensitive, Specific, User‑friendly, Rapid and robust, Equipment‑free, Deliverable) and its updated REASSURED criteria add real‑time connectivity and ease of specimen collection, guiding device design for low‑resource settings. In India, the Indian Council of Medical Research (ICMR) issues detailed guidelines for POCT use, while the Medical Devices Rules, 2017 classify many POCT kits as in‑vitro diagnostic devices requiring registration and compliance with safety standards. Laboratories such as Agam Diagnostics reinforce these mandates through NABL accreditation, which mandates documented quality‑control procedures, regular calibration of analyzers, and competency assessments for operators. Robust quality assurance—encompassing internal controls, lot‑to‑lot verification, and traceability—mitigates pre‑analytical errors, ensures sensitivity and specificity meet WHO thresholds, and supports seamless integration of POCT data into electronic health records for real‑time clinical decision‑making.
Agam Diagnostics: A Model for Integrated POCT Delivery

Agam Diagnostics leverages a free‑home‑collection service that brings patient samples directly to its fully automated laboratory, guaranteeing that most routine panels are reported within 24 hours. This rapid turnaround is reinforced by its dual accreditation – NABL and ICMR – which obliges the lab to meet international quality standards and ensures that point‑of‑care (POCT) results are as reliable as those from central facilities. The laboratory’s workflow bridges centralized high‑throughput automation with bedside POCT technologies; for example, its Vein Finder simplifies phlebotomy, while cartridge‑based immunoassay analyzers deliver on‑site results for cardiac markers, HbA1c, and infectious disease panels. By integrating these devices with a robust digital data pipeline, Agam Diagnostics provides real‑time connectivity to electronic health records, supporting immediate clinical decisions. This model extends diagnostic access to remote Tamil Nadu communities, where patients benefit from home sampling and rapid reporting, and also underpins travel‑related COVID‑19 testing, enabling airport clearance and reducing the need for patients to travel long distances for lab services.
Future Directions: From Decentralized Labs to Smart Health Networks

The next wave of point‑of‑care testing (POCT) will blend AI, cloud connectivity, and home‑based molecular platforms to create a seamless, patient‑centric diagnostic ecosystem. AI‑driven algorithms can automatically interpret POCT outputs—such as cardiac biomarkers, HbA1c, or multiplexed infectious‑disease panels—reducing operator bias and flagging critical values for immediate clinical action. When coupled with tele‑consultation, these AI insights allow clinicians to review results remotely, adjust therapy in real time, and provide patients with instant guidance, an approach already demonstrated by Agam Diagnostics’ integration of digital data pipelines and remote reporting.
Cloud‑based electronic health record (EHR) integration will turn individual POCT results into population‑level intelligence. Continuous upload of de‑identified data to secure servers enables real‑time surveillance of disease trends, supporting rapid public‑health responses to outbreaks such as COVID‑19, influenza, or emerging infections detected by rapid molecular tests. Agam Diagnostics’ existing electronic data infrastructure, aligned with WHO REASSURED criteria, provides a model for how decentralized testing can feed national health dashboards.
Home‑based molecular testing is poised to expand beyond infectious disease detection to include oncology screening. Portable isothermal amplification (LAMP) kits and cartridge‑based PCR devices can deliver pathogen‑specific or cancer‑biomarker results in under an hour, allowing patients in remote Tamil Nadu villages to access early‑stage diagnostics without traveling to a central lab. The combination of lyophilized reagents and smartphone readouts ensures stability in low‑resource settings.
Scaling these innovations requires robust public‑private partnerships. Government initiatives such as India’s Ayushman Bharat and the National Health Policy 2017 can fund device procurement, training, and cold‑chain‑free logistics, while private firms provide technology, AI analytics, and supply‑chain expertise. Collaborative pilots—like those that linked Agam Diagnostics’ home‑collection network with cloud‑enabled POCT devices—demonstrate how shared risk and joint governance can accelerate adoption in underserved areas, ultimately transforming POCT from isolated gadgets into a nationwide smart health network.
The Bottom Line: POCT as a Catalyst for Accessible, High‑Quality Care
Point‑of‑care testing delivers minutes‑scale results, enabling clinicians to treat acute infections, diabetes spikes, or cardiac events during a single visit, which improves outcomes and reduces hospital stay costs. Economically, faster decisions lower repeat‑visit expenses and travel burdens, while societies benefit from broader access in rural and underserved neighborhoods. Agam Diagnostics in Madurai exemplifies this shift, offering NABL‑ and ICMR‑accredited POCT services, home collection, and rapid reporting that extend diagnostics to Tamil Nadu’s remote communities. Clinicians, policymakers, and patients should champion wider POCT adoption, integrate devices into primary‑care pathways, and support regulations to make testing universal.